Facing New Barriers During the COVID-19 Pandemic
April 29, 2020 2024-01-24 18:55Facing New Barriers During the COVID-19 Pandemic

Facing New Barriers During the COVID-19 Pandemic
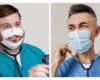
Face masks are a major barrier to reading lips.
The deaf community is facing new barriers as we navigate inaccessible face masks and struggle to follow news broadcasts and teleconferences — but the tools for accessibility are out there
As originally posted in Business Insider
- Sarah Katz is a freelance writer who covers the intersection between disability and mental health, relationships, entertainment, and public services.
- As a deaf individual, the coronavirus pandemic has been particularly difficult for her to navigate — people wearing masks obstructing their lips presents major barriers to communication.
- Some deaf individuals have faced difficulty in healthcare — many are no longer allowed to use in-person interpreters.
- Teleconferencing software’s auto-captioning can be unreliable and error-filled, making it less accessible to the hard of hearing.
- Visit Business Insider’s homepage for more stories.
Since President Trump declared a national emergency due to the COVID-19 outbreak over a month ago, I have communicated in person with only one individual outside my home: the pharmacist who handed me my prescription from the drive-through window.
Only I couldn’t really communicate with the pharmacist, because I am deaf and couldn’t read their lips through the opaque white surgical mask. Still, after a laborious exchange in which I used gestures and the little residual hearing I have, I valiantly left with what I came for.
While the outbreak has upended life for everyone, deaf and hard of hearing individuals like me have encountered significant barriers to communication during this crisis. This should come as no surprise, since research shows that deaf and hard of hearing people in the United States are largely underserved during emergencies. It’s deplorable, though: 48 million Americans are deaf and hard of hearing, and several federal laws mandate our protection during emergencies — but everyone keeps forgetting we exist. It’s time for this country to establish a comprehensive set of national guidelines that enable state and local governments to provide access to emergency services for deaf and hard of hearing people before, during, and after a crisis.
For one, inaccessible face masks shouldn’t be the standard. They hinder speechreading and present barriers for deaf and hard of hearing individuals who use American Sign Language (ASL) or Cued American English via Cued Speech (CS), a visual mode of communication that disambiguates speechreading. ASL grammar is displayed on the face, while CS uses handshapes, placements, and mouth movements. Both require facial expression to supply meaning and tone that would otherwise be conveyed through speech, which inaccessible masks hide.
But, lest you think they’re a necessary evil, accessible face masks do exist. Safe’N’Clear, Inc., a company that develops surgical masks, has created a mask with an FDA-approved, fog-resistant transparent window to facilitate clear and unrestricted communication.
Clear masks could make everyone happier in the long run. Safe’N’Clear founder and Chief Executive Officer Dr. Anne McIntosh told Business Insider that, while the “The Communicator” mask does benefit people who are deaf and hard of hearing, her invention helps everyone communicate more effectively.
“The human smile is such a NECESSARY part of our ability to connect with others, especially when social distancing says we cannot hug, shake hands, kiss, or wrap our arms around another person’s shoulder,” she wrote in an email. “As social beings, we need to feel ‘connected’ and ‘in relationships’ with others and the smile is our way to communicate ‘community’ to others.”
In addition to making it harder for millions of deaf Americans to communicate, opaque masks are harming their mental health. Several deaf individuals have told me that the prevalence of masks triggers significant anxiety, to the point where they avoid leaving their homes altogether for essential activities, such as grocery shopping.
“I’ve had my husband do all the shopping and errands for us,” said Courtney Poole, a deaf home health care manager in Locust, North Carolina, “mainly due to my fear of not being able to talk to or understand anyone wearing masks and standing far away. Basically, I don’t want to deal with it.”
The barriers transcend face masks: As confirmed cases of the coronavirus overwhelm hospitals, deaf and hard of hearing patients are reporting inadequate accommodations in hospital settings.
For example, many medical professionals are treating patients from behind a barrier and not allowing in-person interpreters. On April 16, The Los Angeles Times reported that Jennylee Bruno, a deaf author and mother of five, received an American Sign Language interpreter over video conferencing software, but the feed froze multiple times while Bruno received her feared diagnosis of COVID-19, heightening her anxiety.
“I feel like they were giving me a death sentence,” she told the Times. “I wanted to ask, am I going to die, what can we do, is there a cure, what about medications, what’s the plan?”
Sandi Sinnott, a deaf Navy retiree in Havelock, North Carolina, shared a similarly horrifying story. She told Business Insider that she went to the local emergency room in March for a “simple CT scan” for pneumonia and ended up hospitalized for a week with only choppy video access to a remote interpreter. She said that she was not told why she was admitted, adding, “I believe they said as little as possible because of communication barriers.”
Sinnott also said that she was not initially tested for COVID-19, because she didn’t have a fever; however, she later received a test that came back negative.
Deaf and hard of hearing individuals are also reporting unsatisfactory access to information about the outbreak.
“Many government press briefings were not accessible to deaf and hard of hearing people, and to address this issue, we have been focused on advocating for American Sign Language (ASL) interpreters and accurate captioning in all broadcasts of such emergency briefings,” said the National Association of the Deaf’s Chief Executive Officer Howard Rosenblum. “We have received many complaints from deaf and hard of hearing people unable to understand from the briefings what they are supposed to do or avoid to stay safe and healthy, and we have given them tools to advocate for their communication access.”
Rosenblum explained that while live national broadcasts must provide captioning under federal law, live news broadcasts from local new stations aren’t required to provide captioning and are “only live captioned in the top 25 markets.” Those that do provide captioning are “usually” not accurate, he said, “as most of them recycle the teleprompter script as captioning, and that does not include breaking news which is what most emergency broadcasts entail.”
Calls for social distancing have also affected deaf and hard of hearing people in many other areas, including in K-12 education, universities, workplaces, and courtrooms. While teleconferencing platforms enable many people to continue learning and working from home, many don’t know that auto-captioning through these platforms is often unreliable and riddled with errors, which makes it all the more important that those in positions of power employ truly inclusive measures informed by the realities faced by the deaf community.
To address these problems, the NAD is urging all government agencies to implement the recommendations detailed in their emergency communication position statement, and for hospitals to utilize their guidelines. The NAD and other advocates have also created a guide for deaf and hard of hearing individuals who may need to visit the hospital.
Experts and resources on disability-inclusive emergency management abound. It’s time to use them before it’s too late.
Purchase Online
Featured Deaf Leader
Recent Articles